Bisotrak Tablets 5mg
Therapy Area
Cardiology
1.0 Generic name
Bisoprolol Fumarate Tablet 2.5mg/5mg
2.0 Qualitative and quantitative composition
Each film-coated tablet contains:
Bisoprolol Fumarate 2.5 mg/5 mg
3.0 Dosage form and strength
Film-coated tablet, Bisoprolol Fumarate 2.5 mg/5 mg
4.0 Clinical particulars
4.1 Therapeutic indication
BisotrakTM is indicated for the treatment of hypertension, coronary heart disease (angina pectoris), congestive heart failure (CHF).
4.2 Posology and method of administration
Treatment of hypertension and chronic stable angina pectoris:
Adults
The dosage should be individually adjusted. It is recommended to start with 5 mg per day. The usual dose is 10 mg once daily with a maximum recommended dose of 20 mg per day.
Renal impairment
In patients with severe renal impairment (creatinine clearance < 20 ml/min) the dose should not exceed 10 mg once daily. This dosage may eventually be divided into halves.
Severe hepatic impairment
No dosage adjustment is required; however careful monitoring is advised.
Elderly
No dosage adjustment is normally required. It is recommended to start with the lowest possible dose.
Pediatric population
There is no experience with bisoprolol in children, therefore its use cannot be recommended for children.
Discontinuation of treatment
Treatment should not be stopped abruptly. The dosage should be diminished slowly by a weekly halving of the dose.
Treatment of stable chronic heart failure
Adults
Standard treatment of CHF consists of an ACE inhibitor (or an angiotensin receptor blocker in case of intolerance to ACE inhibitors), a beta-blocking agent, diuretics, and when appropriate cardiac glycosides. Patients should be stable (without acute failure) when bisoprolol treatment is initiated.
It is recommended that the treating physician should be experienced in the management of chronic heart failure.
Transient worsening of heart failure, hypotension, or bradycardia may occur during the titration period and thereafter.
Titration phase
The treatment of stable chronic heart failure with bisoprolol requires a titration phase.
The treatment with bisoprolol is to be started with a gradual up titration according to the following steps:
1.25 mg once daily for 1 week, if well tolerated increase to
2.5 mg once daily for a further week, if well tolerated increase to
3.75 mg once daily for a further week, if well tolerated increase to
5 mg once daily for the 4 following weeks, if well tolerated increase to
7.5 mg once daily for the 4 following weeks, if well tolerated increase to
10 mg once daily for the maintenance therapy.
The maximum recommended dose is 10 mg once daily.
Close monitoring of vital signs (heart rate, blood pressure) and symptoms of worsening heart failure is recommended during the titration phase. Symptoms may already occur within the first day after initiating the therapy.
Treatment modification
If the maximum recommended dose is not well tolerated, gradual dose reduction may be considered.
In case of transient worsening of heart failure, hypotension, or bradycardia reconsideration of the dosage of the concomitant medication is recommended. It may also be necessary to temporarily lower the dose of bisoprolol or to consider discontinuation.
The reintroduction and/or up titration of bisoprolol should always be considered when the patient becomes stable again.
If discontinuation is considered, gradual dose decrease is recommended, since abrupt withdrawal may lead to acute deterioration of the patient’s condition.
Treatment of stable chronic heart failure with bisoprolol is generally a long-term treatment.
Special population
Hepatic or Renal impairment
There is no information regarding pharmacokinetics of bisoprolol in patients with chronic heart failure and with impaired hepatic or renal function. Up titration of the dose in these populations should therefore be made with additional caution.
Elderly
No dosage adjustment is required.
Pediatric population
There is no experience with bisoprolol in children, therefore its use cannot be recommended for children.
Method of administration
For oral use
Bisoprolol tablets should be taken in the morning and can be taken with food. They should be swallowed with liquid and should not be chewed.
4.3 Contraindications
Bisoprolol is contra-indicated in chronic heart failure patients with:
- hypersensitivity to the active substance
- acute heart failure or during episodes of heart failure decompensation requiring i.v. inotropic therapy
- cardiogenic shock
- Second or third degree AV block (without a pacemaker)
- sick sinus syndrome
- sinoatrial block
- symptomatic bradycardia
- symptomatic hypotension
- severe bronchial asthma or severe chronic obstructive pulmonary disease
- severe forms of peripheral arterial occlusive disease or severe forms of Raynaud's syndrome
- untreated phaeochromocytoma
- metabolic acidosis
4.4 Special warnings and Precautions
Special Warnings
Applies only to chronic heart failure:
The treatment of stable chronic heart failure with bisoprolol has to be initiated with a special titration phase
Applies to all indications:
Especially in patients with ischaemic heart disease the cessation of therapy with bisoprolol must not be done abruptly unless clearly indicated, because this may lead to transitional worsening of heart condition.
Precautions
Applies only to hypertension or angina pectoris:
Bisoprolol must be used with caution in patients with hypertension or angina pectoris and accompanying heart failure.
Applies only to chronic heart failure:
The initiation of treatment of stable chronic heart failure with bisoprolol necessitates regular monitoring.
There is no therapeutic experience of bisoprolol treatment of heart failure in patients with the following diseases and conditions:
- insulin dependent diabetes mellitus (type I)
- severely impaired renal function
- severely impaired hepatic function
- restrictive cardiomyopathy
- congenital heart disease
- hemodynamically significant organic valvular disease
- myocardial infarction within 3 months
Applies to all indications:
Bisoprolol must be used with caution in:
- bronchospasm (bronchial asthma, obstructive airways diseases). In bronchial asthma or other chronic obstructive lung diseases, which may cause symptoms, bronchodilating therapy is recommended to be given concomitantly. Occasionally an increase of the airway resistance may occur in patients with asthma, therefore the dose of beta 2 stimulants may have to be increased.
- diabetes mellitus with large fluctuations in blood glucose values; symptoms of hypoglycaemia (e.g. tachycardia, palpitations or sweating) can be masked
- strict fasting
- ongoing desensitisation therapy. As with other beta-blockers, bisoprolol may increase both the sensitivity towards allergens and the severity of anaphylactic reactions. Epinephrine treatment does not always yield the expected therapeutic effect.
- First degree AV block
- Prinzmetal's angina; Cases of coronary vasospasm have been observed. Despite its high beta1-selectivity, angina attacks cannot be completely excluded when bisoprolol is administered to patients with Prinzmetal's angina.
- peripheral arterial occlusive disease. Aggravation of symptoms may occur especially when starting therapy.
- general anaesthesia
In patients undergoing general anaesthesia beta-blockade reduces the incidence of arrhythmias and myocardial ischemia during induction and intubation and the post-operative period. It is currently recommended that maintenance beta-blockade be continued peri-operatively. The anaesthetist must be aware of beta-blockade because of the potential for interactions with other drugs, resulting in bradyarrhythmias, attenuation of the reflex tachycardia and the decreased reflex ability to compensate for blood loss. If it is thought necessary to withdraw beta-blocker therapy before surgery, this should be done gradually and completed about 48 hours before anaesthesia.
Combination of bisoprolol with calcium antagonists of the verapamil or diltiazem type, with Class I antiarrhythmic drugs and with centrally acting antihypertensive drugs is generally not recommended.
Although cardioselective (beta1) beta-blockers may have less effect on lung function than non-selective beta-blockers, as with all beta-blockers, these should be avoided in patients with obstructive airways diseases, unless there are compelling clinical reasons for their use. Where such reasons exist, bisoprolol may be used with caution. In patients with obstructive airways diseases, the treatment with bisoprolol should be started at the lowest possible dose and patients should be carefully monitored for new symptoms (e.g. dyspnea, exercise intolerance, cough). In bronchial asthma or other chronic obstructive lung diseases, which may cause symptoms, bronchodilating therapy should be given concomitantly. Occasionally an increase of the airway resistance may occur in patients with asthma, therefore the dose of beta2-stimulants may have to be increased.
Patients with psoriasis or with a history of psoriasis should only be given beta-blockers (e.g. bisoprolol) after carefully balancing the benefits against the risks.
In patients with phaeochromocytoma bisoprolol must not be administered until after alpha-receptor blockade.
Under treatment with bisoprolol the symptoms of a thyrotoxicosis may be masked
4.5 Drug interactions
Combinations not recommended
Applies only to chronic heart failure:
Class-I antiarrhythmic drugs (e.g. quinidine, disopyramide, lidocaine, phenytoin, flecainide, propafenone): effect on atrio-ventricular conduction time may be potentiated and negative inotropic effect increased.
Applies to all indications:
Calcium antagonists of the verapamil type and to a lesser extent of the diltiazem type: negative effect on contractility and atrio-ventricular conduction. Intravenous administration of verapamil in patients on beta-blocker treatment may lead to profound hypotension and atrio-ventricular block.
Centrally-acting antihypertensive drugs (e.g. clonidine, methyldopa, moxonidine, rilmenidine): concomitant use of centrally-acting antihypertensive drugs may further decrease the central sympathetic tonus and may thus lead to reduction of heart rate and cardiac output and to vasodilatation. Abrupt withdrawal, particularly if prior to beta-blocker discontinuation, may increase the risk of “rebound hypertension”.
Combinations to be used with caution
Applies only to hypertension or angina pectoris:
Class-I antiarrhythmic drugs (e.g. quinidine, disopyramide; lidocaine, phenytoin; flecainide propafenone): Effect on atrioventricular conduction time may be potentiated and negative inotropic effect increased.
Applies to all indications
Calcium antagonists of the dihydropyridine type such as felodipine and amlodipine: Concomitant use may increase the risk of hypotension, and an increase in the risk of a further deterioration of the ventricular pump function in patients with heart failure cannot be excluded.
Class-III antiarrhythmic drugs (e.g. amiodarone): Effect on atrio-ventricular conduction time may be potentiated.
Parasympathomimetic drugs: Concomitant use may increase atrio-ventricular conduction time and the risk of bradycardia.
Topical beta-blocking agents (e.g. eye drops for glaucoma treatment) may add to the systemic effects of bisoprolol.
Insulin and oral antidiabetic drugs: Increase of blood sugar lowering effect. Blockade of beta-adrenoreceptors may mask symptoms of hypoglycaemia.
Anaesthetic agents: Attenuation of the reflex tachycardia and increase of the risk of hypotension
Digitalis glycosides: Increase of atrio-ventricular conduction time, reduction in heart rate.
Non-steroidal anti-inflammatory drugs (NSAIDs): NSAIDs may reduce the hypotensive effect of bisoprolol.
β -Sympathomimetic agents (e.g. isoprenaline, dobutamine): Combination with bisoprolol may reduce the effect of both agents.
Sympathomimetics that activate both β - and α -adrenoceptors (e.g. norepinephrine, epinephrine): Combination with bisoprolol may unmask the α -adrenoceptor-mediated vasoconstrictor effects of these agents leading to blood pressure increase and exacerbated intermittent claudication. Such interactions are considered to be more likely with nonselective β -blockers.
Concomitant use with antihypertensive agents as well as with other drugs with blood pressure lowering potential (e.g. tricyclic antidepressants, barbiturates, phenothiazines) may increase the risk of hypotension.
Combinations to be considered
Mefloquine: increased risk of bradycardia
Monoamine oxidase inhibitors (except MAO-B inhibitors): Enhanced hypotensive effect of the beta-blocking agents but also risk for hypertensive crisis.
Rifampicin: Slight reduction of the half-life of bisoprolol possible due to the induction of hepatic drug metabolizing enzymes. Normally no dosage adjustment is necessary.
Ergotamine derivatives: Exacerbation of peripheral circulatory disturbances.
4.6 Use in special populations
Pregnancy
Bisoprolol has pharmacological effects that may cause harmful effects on pregnancy and/or the fetus/newborn. In general, beta-adrenoceptor blocking agents reduce placental perfusion, which has been associated with growth retardation, intrauterine death, abortion or early labour. Adverse effects (e.g. hypoglycaemia and bradycardia) may occur in the fetus and newborn infant. If treatment with beta-adrenoceptor blocking agents is necessary, beta1-selective adrenoceptor blocking agents are preferable.
Bisoprolol is not recommended during pregnancy unless clearly necessary. If treatment with bisoprolol is considered necessary, the uteroplacental blood flow and fetal growth should be monitored. In case of harmful effects on pregnancy or the fetus alternative treatment should be considered. The newborn infant must be closely monitored. Symptoms of hypoglycaemia and bradycardia are generally to be expected within the first 3 days.
Breast-feeding
There are no data on the excretion of bisoprolol in human breast milk or the safety of bisoprolol exposure in infants. Therefore, breastfeeding is not recommended during administration of bisoprolol.
4.7 Effects on the ability to drive and use machines
In a study with coronary heart disease patients, bisoprolol did not impair driving performance. However, depending on the individual patient’s response to treatment an effect on the ability to drive a vehicle or to use machines cannot be excluded. This needs to be considered particularly at start of treatment, upon change of medication, or in conjunction with alcohol.
4.8 Undesirable effects
The following definitions apply to the frequency terminology used hereafter:
Very common (≥ 1/10)
Common (≥ 1/100 to 1/10)
Uncommon (≥ 1/1,000 to 1/100)
Rare (≥ 1/10,000, to 1/1,000)
Very rare (< 1/10,000)
Not known (cannot be estimated from the available data)
Psychiatric disorders:
Uncommon: sleep disorders, depression.
Rare: nightmares, hallucinations.
Nervous system disorders:
Common: dizziness*, headache*.
Rare: syncope
Eye disorders:
Rare: reduced tear flow (to be considered if the patient uses lenses).
Very rare: conjunctivitis.
Ear and labyrinth disorders:
Rare: hearing disorders
Cardiac disorders:
Very common: bradycardia (in patients with chronic heart failure).
Common: worsening of pre-existing heart failure (in patients with chronic heart failure).
Uncommon: AV-conduction disturbances, worsening of pre-existing heart failure (in patients with hypertension or angina pectoris) ; bradycardia (in patients with hypertension or angina pectoris).
Vascular disorders:
Common: feeling of coldness or numbness in the extremities, hypotension especially in patient with heart failure.
Uncommon: orthostatic hypotension.
Respiratory, thoracic and mediastinal disorders:
Uncommon: bronchospasm in patients with bronchial asthma or a history of obstructive airways disease.
Rare: allergic rhinitis.
Gastrointestinal disorders:
Common: gastrointestinal complaints such as nausea, vomiting, diarrhoea, constipation.
Hepatobiliary disorders:
Rare: hepatitis.
Skin and subcutaneous tissue disorders:
Rare: hypersensitivity reactions (pruritus, flush, rash and angioedema).
Very rare: betablockers may provoke or worsen psoriasis or induce psoriasislike rash, alopecia.
Musculoskeletal and connective tissue disorders:
Uncommon: muscular weakness and cramps.
Reproductive system and breast disorders:
Rare: erectile dysfunction.
General disorders:
Common: asthenia (in patients with chronic heart failure), fatigue*.
Uncommon: asthenia (in patients with hypertension or angina pectoris)
Investigations:
Rare: increased triglycerides, increased liver enzymes (ALAT, ASAT). Applies only to hypertension or angina pectoris: *These symptoms especially occur at the beginning of the therapy. They are generally mild and usually disappear within1-2 weeks.
Reporting of side effects
Reporting suspected adverse reactions after authorisation of the medicinal product is important. It allows continued monitoring of the benefit/risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions via email to: medico@zuventus.com
Website: https://www.zuventus.com/drug-safety-reporting
By reporting side effects, you can help provide more information on the safety of this medicine.
4.9 Overdose
Symptoms
The most common signs expected with overdose of a beta-blocker are bradycardia, hypotension, bronchospasm, acute cardiac insufficiency and hypoglycaemia. There is limited experience with overdose of bisoprolol, only a few cases of overdose with bisoprolol have been reported. Bradycardia and/or hypotension were noted. All patients recovered. There is a wide inter-individual variation in sensitivity to one single high dose of bisoprolol and patients with heart failure are probably very sensitive.
Management
In general, if overdose occurs, discontinuation of bisoprolol treatment and supportive and symptomatic treatment is recommended.
Based on the expected pharmacologic actions and recommendations for other beta-blocking agents, the following general measures should be considered when clinically warranted.
Bradycardia: Administer intravenous atropine. If the response is inadequate, isoprenaline or another agent with positive chronotropic properties may be given cautiously. Under some circumstances, transvenous pacemaker insertion may be necessary.
Hypotension: Intravenous fluids and vasopressors should be administered. Intravenous glucagon may be useful.
AV block (second or third degree): Patients should be carefully monitored and treated with isoprenaline infusion or temporary pacing.
Acute worsening of heart failure: Administer i.v. diuretics, inotropic agents, vasodilating agents.
Bronchospasm: Administer bronchodilator therapy such as isoprenaline, beta 2 -sympathomimetic drugs and/or aminophylline.
Hypoglycaemia: Administer i.v. glucose.
Limited data suggest that bisoprolol is hardly dialysable.
5.0 Pharmacological properties
5.1 Mechanism of Action
Bisoprolol is a potent highly beta 1 -selective-adrenoceptor blocking agent, lacking intrinsic sympathomimetic and relevant membrane stabilising activity. It only shows low affinity to the beta 2 -receptor of the smooth muscles of bronchi and vessels as well as to the beta 2 -receptors concerned with metabolic regulation. Therefore, bisoprolol is generally not to be expected to influence the airway resistance and beta 2 -mediated metabolic effects. Its beta 1 -selectivity extends beyond the therapeutic dose range.
5.2 Pharmacodynamic properties
Hypertension or angina pectoris:
Bisoprolol is used for the treatment of hypertension and angina pectoris. As with other Beta1blocking agents, the method of acting in hypertension is unclear. However, it is known that Bisoprolol reduces plasma renin activity markedly.
Antianginal mechanism: Bisoprolol by inhibiting the cardiac beta receptors inhibits the response given to sympathetic activation. That results in the decrease of heart rate and contractility this way decreasing the oxygen demand of the cardiac muscle.
In acute administration in patients with coronary heart disease without chronic heart failure bisoprolol reduces the heartrate and stroke volume and thus the cardiac output and oxygen consumption. In chronic administration the initially elevated peripheral resistance decreases.
5.3 Pharmacokinetics
Absorption
Bisoprolol is absorbed almost completely from the gastrointestinal tract. Together with the very small first pass effect in the liver, this results in a high bioavailability of approximately 90%. The plasma protein binding of bisoprolol is about 30%. The distribution volume is 3.5 l/kg. The total clearance is approximately 15 l/h.
Distribution
The plasma elimination half-life (10-12 hours) provides 24 hours’ efficacy following a once daily dosage.
Biotransformation and Elimination
Bisoprolol is excreted from the body by two routes. 50% is metabolized by the liver to inactive metabolites which are then excreted by the kidneys. The remaining 50% is excreted by the kidneys in an unmetabolised form. Since the elimination takes place in the kidneys and the liver to the same extent a dosage adjustment is not required for patients with impaired liver function or renal insufficiency.
Special population
In patients with chronic heart failure (NYHA stage III) the plasma levels of bisoprolol are higher and the half-life is prolonged compared to healthy volunteers. Maximum plasma concentration at steady state is 64± 21 ng/ml at a daily dose of 10 mg and the half-life is 17± 5 hours.
6.0 Nonclinical properties
6.1 Animal Toxicology or Pharmacology
Preclinical data reveal no special hazard for humans based on conventional studies of safety pharmacology, repeated dose toxicity, genotoxicity or carcinogenicity. Like other beta-blocking agents, bisoprolol caused maternal (decreased food intake and decreased body weight) and embryo/fetal toxicity (increased incidence of resorptions, reduced birthweight of the offspring, retarded physical development) at high doses but was not teratogenic.
7.0 Description
Bisoprolol fumarate is a synthetic, beta1-selective (cardio-selective) adrenoceptor blocking agent.
Bisoprolol fumarate:
Chemical Name : s (±)-1-[4-[[2-(1-Methylethoxy)ethoxy] methyl] phenoxy] -3-[(1-methylethyl) amino] -2-propanol (E)-2-butenedioate (2:1) (salt)
Molecular formula: (C18H31NO4)2.C4H4O4
Molecular weight : 766.97
Chemical structure:
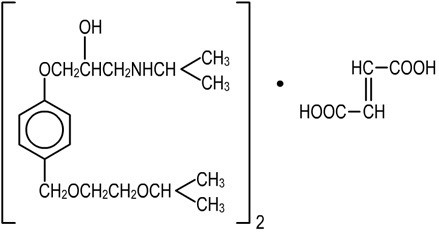
8.0 Pharmaceutical particulars
8.1 Incompatibilities
Not applicable
8.2 Shelf life
Refer to the pack.
8.3 Packaging Information
BisotrakTM 2.5mg: 10 tablets per Blister strips
BisotrakTM 5mg: 10 tablets per Blister strips
8.4 Storage and handling instructions
Store below 300C.
Protect from light and moisture.
9.0 Patient counselling information
Patients, especially those with coronary artery disease, should be warned about discontinuing use of BisotrakTM without a physician’s supervision. Patients should also be advised to consult a physician if any difficulty in breathing occurs, or if they develop signs or symptoms of congestive heart failure or excessive bradycardia.
Patients subject to spontaneous hypoglycemia, or diabetic patients receiving insulin or oral hypoglycemic agents, should be cautioned that beta-blockers may mask some of the manifestations of hypoglycemia, particularly tachycardia, and bisoprolol fumarate should be used with caution. Patients should know how they react to this medicine before they operate automobiles and machinery or engage in other tasks requiring alertness.
11.0 Date of revision of the text
This leaflet was last revised in June 2024.
About leaflet
Read all of this leaflet carefully before you start taking this medicine because it contains important information for you.
- Keep this leaflet. You may need to read it again.
- If you have any further questions, ask your doctor or pharmacist.
- This medicine has been prescribed for you. Do not pass it on to others. It may harm them, even if their signs of illness are the same as yours.
- If you get any side effects, talk to your doctor or pharmacist. This includes any possible side effects not listed in this leaflet. See section 4.
What is in this leaflet
- What BisotrakTM is and what it is used for
- What you need to know before you take BisotrakTM
- How to take BisotrakTM
- Possible side effects
- How to store BisotrakTM
- Contents of the pack and other information
1. What BisotrakTM is and what it is used for
The active substance in BisotrakTM is Bisoprolol fumarate. Bisoprolol belongs to a group of medicines called beta-blockers. Beta-blocker protects heart from too much activity. This medicine works by affecting the body’s response to some nerve impulses, especially in the heart. As a result, Bisoprolol fumarate slows down the heart rate and makes the heart more efficient at pumping blood around the body. Heart failure occurs when the heart muscle is weak and unable to pump enough blood to supply the body’s need. Bisoprolol tablets are used in combination with other medicines to treat stable heart failure. It is used to treat high blood pressure (hypertension) and angina pectoris (chest pain caused by blockages in the arteries that supply the heart muscle).
2. What you need to know before you take BisotrakTM
Do not take Bisoprolol Fumarate if you:
- are allergic to bisoprolol fumarate
- have severe asthma or severe chronic lung disease
- have a slow or irregular heart rate. Ask your doctor if you are not sure
- have very low blood pressure
- have severe blood circulation problems (such as Raynaud’s syndrome), which may cause your fingers and toes to tingle or turn pale or blue
- have heart failure that suddenly becomes worse and/ or may require hospital treatment
- Cardiogenic shock, which is an acute serious heart condition causing low blood pressure and circulatory failure.
- have excess acid in the blood, a condition known as metabolic acidosis
- have untreated phaeochromocytoma, a rare tumour of the adrenal gland (medulla)
Tell your doctor if you are not sure about any of the above: your doctor will be able to advise you.
Warnings and precautions
Talk to your doctor or pharmacist before taking Bisoprolol Fumarate. He or she may want to take special care (for example give additional treatment or perform more frequent checks) if you have any of the following conditions if you:
- have asthma or chronic lung disease
- have diabetes. Bisoprolol fumarate can hide the symptoms of low blood sugar
- are fasting from solid food
- are treated for hypersensitivity (allergic) reactions. Bisoprolol may make your allergy worse or often difficult to treat.
- have certain heart disease such as disturbance in heart rhythm or severe chest pain at rest (Prinzmetal’s angina)
- have any liver or kidney problems
- have any problems with the circulation in your limbs
- are taking verapamil or diltiazem, medicines used to treat heart conditions. Concomitant use is not recommended, see also “taking other medicines”
- have (or have had) psoriasis (a recurring skin rash)
- have phaeochromocytoma (tumour of the adrenal gland). Your doctor will need to treat this before prescribing bisoprolol for you
- have a thyroid problem. The tablets can hide symptoms of an overactive thyroid
Consult your doctor if one of the above warnings is applicable to you, or has been in the past.
In addition, tell your doctor if you are going to have:
- Desensitization therapy (for example for the prevention of hay fever), because Bisoprolol fumarate may make it more likely that you experience as allergic reaction or such reaction may be more severe.
- Anesthesia (for example for surgery) because this medicine may influence how your body react to this situation.
Children and adolescents
Bisoprolol fumarate is not recommended for use in children or adolescents.
Other medicines and Bisoprolol Fumarate
Tell your doctor or pharmacist if you are taking, have recently taken or might take any other medicines. Certain medicines cannot be used at the same time, while other drugs require specific changes (to the dose, for example).
Do not take the following medicines with Bisoprolol Fumarate without special advice from your doctor:
- Medicines for controlling the blood pressure or medicines for heart problems (such as amiodarone, amlodipine, clonidine, digitalis glycosides, diltiazem, disopyramide, felodipine, flecainide, lidocaine, methyldopa, moxonidine, phenytoin, propafenone, quinidine, rilmenidine, verapamil)
- Medicines for depression e.g. imipramine, amitriptyline, moclobemide
- Medicines to treat mental illness e.g. phenothiazines such as levomepromazine
- Medicines used for anaesthesia during an operation (see also “Warnings and precautions”)
- Medicines used to treat epilepsy e.g. barbiturates such as phenobarbital
- Certain pain killers (for instance acetyl salicylic acid, diclofenac, indomethacin, ibuprofen, naproxen)
- Medicines for asthma or medicines used for a blocked nose
- Medicines used for certain eye disorders such as glaucoma (increased pressure in the eye) or used to widen the pupil of the eye.
- Certain medicines to treat clinical shock (e. g. adrenaline, dobutamine, noradrenaline)
- Mefloquine, a medicine for malaria
All these drugs as well as bisoprolol may influence the blood pressure and/or heart function.
- Rifampicin for the treatment of infections
- medicines to treat severe headaches or migraines (ergotamine derivatives).
It is also especially important to speak with your doctor if you are taking:
- Insulin or other products for diabetes. The blood glucose reducing effect may be enhanced. Symptoms of low blood glucose level can be masked.
Bisoprolol Fumarate with food, drink and alcohol
Bisoprolol Fumarate may be taken with or without food and should be swallowed whole with a drink of water.
Pregnancy, breast-feeding and fertility
Do not take bisoprolol if you are pregnant or may be pregnant. Bisoprolol Fumarate may be harmful to the pregnancy and/or the unborn child. There is an increased possibility of premature birth, miscarriage, low blood sugar level and reduced heart rate of the child. The growth of the baby may also be affected. It is not known if bisoprolol is excreted in the breast milk and therefore it is not recommended while breast-feeding. If you are pregnant or breast-feeding, think you may be pregnant or are planning to have a baby, ask your doctor or pharmacist for advice before taking any medicine.
Driving and using machines
These tablets may make you feel tired, drowsy or dizzy. If you suffer from these side effects, do not operate vehicles and/or machines. Be aware of the possibility of these effects, particularly at the beginning of the treatment, with changes in medication and with use in combination with alcohol.
3. How to take BisotrakTM
Always take this medicine exactly as your doctor or pharmacist has told you. Check with your doctor or pharmacist if you are not sure. Treatment with Bisoprolol fumarate tablet requires regular medical check up. This is particularly important in the initiation of therapy and during dose increase. Bisoprolol fumarate tablet should be taken in the morning, with or without food. Swallow the tablet whole with some water and do not chew or crush them. The tablet can be divided into equal doses. Treatment with Bisoprolol fumarate tablet is usually prolonged.
Adult:
Chest pain and high blood pressure:
Your doctor will start the treatment with lowest possible dose (5 mg). Your doctor will monitor you closely at the start of treatment. Your doctor will increase your dose to obtain the best possible dosage for you.
The maximum recommended dose is 20 mg once per day.
Patient with kidney disease:
Patient with severe kidney disease should not exceed 10 mg of bisoprolol once daily. Please consult your doctor before starting to use this medicine.
Patient with liver disease:
Patient with severe liver disease should not exceed 10 mg of bisoprolol once daily. Please consult your doctor before starting to use this medicine.
Heart failure:
Before you start using Bisoprolol Fumarate you should already be taking other medicines for heart failure including an ACE-inhibitor, a diuretic and (as an added option) a cardiac glycoside.
The dose of Bisoprolol Fumarate will be increased gradually until the dose that is suitable for you has been found:
Treatment with Bisoprolol fumarate tablet must be started at a low dose and increased gradually. Your doctor will decide how to increase the dose, and this will normally be done in the following way:
Adults and elderly: the recommended dose is
1.25 mg once daily for 1 week. If this is well tolerated, the dose may be increased to:
2.5 mg once daily during the next week. If this is well tolerated, the dose may be increased to:
3.75 mg once daily during the next week. If this is well tolerated, the dose may be increased to:
5 mg once daily during the next 4 weeks. If this is well tolerated, the dose may be increased to:
7.5 mg once daily during the next 4 weeks. If this is well tolerated, the dose may be increased to:
10 mg once daily as a maintenance dose.
Maximum dose: once daily 10 mg.
Depending on how well you tolerate the medicine, your doctor may also decide to lengthen the time between dose increases. If your condition gets worse or you no longer tolerate the drug, it may be necessary to reduce the dose again or to interrupt treatment. In some patients a maintenance dose lower than 10 mg bisoprolol may be sufficient.
Your doctor will tell you what to do.
If you have to stop treatment entirely, your doctor will usually advice you to reduce the dose gradually, as otherwise your condition may become worse.
Your heart rate and blood pressure will be monitored closely as the dose is increased.
Patients with liver or kidney problems:
Your doctor will take extra care when adjusting the dose of Bisoprolol Fumarate.
Use in children and adolescents:
Bisoprolol Fumarate is not recommended for use in children or adolescents.
Elderly patient:
In general adjustment of the dose is not needed. It is recommended to start with lowest possible dose.
If you notice that the effect of Bisoprolol Fumarate is too strong or not strong enough, please consult your doctor or pharmacist.
Duration of the treatment
Bisoprolol Fumarate will usually be used long-term.
The tablet can be divided into equal halves
If you take more Bisoprolol Fumarate than you should
If you have accidentally taken more than the prescribed dose, tell your doctor/pharmacist immediately. Take any remaining tablets or this leaflet with you so the medical staff know exactly what you have taken. Symptoms of overdose may include dizziness, light-headedness, fatigue, breathlessness and/or wheezing. Also, there may be reduced heart rate, reduced blood pressure, insufficient action of the heart and a low blood glucose level (which may involve feelings of hunger, sweating and palpitations).
If you forget to take Bisoprolol Fumarate
Do not take a double dose to make up for a forgotten dose. Take the normal dose as soon as you remember and then carry on with the usual dose the next day. If you stop taking Bisoprolol Fumarate Treatment with Bisoprolol Fumarate must not be stopped abruptly. If you suddenly stop taking this medicine your condition may get worse. The dose of bisoprolol must be reduced gradually over a few weeks as advised by your doctor.
If you have any further questions on the use of this medicine, ask your doctor or pharmacist.
4. Possible side effects
Like all medicines, this medicine can cause side effects, although not everybody gets them.
To prevent serious reaction, speak to a doctor immediately if a side effect is severe, occurs suddenly or gets worse rapidly. The most serious side effects are related to the heart function:
- Slowing of heart rate (affect more than 1 patient in 10 in patient with chronic heart failure and affected less than 1 patient in 100 in patient with hypertension or angina pectoris)
- Worsening of heart failure (affects more than 1 patient in 100 in patient with chronic heart failure and affected less than 1 patient in 100 in patient with hypertension or angina pectoris)
- irregular heartbeat (affects less than 1 patient in 100)
- Worsening of symptom of blockage of the main blood vessel to the legs, especially at the start of treatment (Frequency not stated).
If you feel dizzy or weak or have breathing difficulties, please contact your doctor as soon as possible.
Further side effects are listed below according to how frequently they may occur:
Common (may affect up to 1 in 10 people):
- Tiredness*, feeling weak, (In patient with chronic heart failure), dizziness*, headache*
- Feeling of coldness or numbness in hands or feet
- low blood pressure, especially in patient with heart failure.
- Stomach or intestine problem such as nausea, vomiting, diarrhoea or constipation
Uncommon (may affect up to 1 in 100 people):
- Sleep disturbances
- Depression
- Breathing problems in patients with asthma or chronic lung disease
- Muscle weakness, muscle cramps
- feeling weak (In patient with hypertension or angina pectoris)
Rare: (may affect up to 1 in 1,000 people):
- Hearing problems
- Inflammation of the lining of the nose, causing a runny nose with irritation
- Allergic reactions (itching, flushed appearance, rash). You should see your doctor straight away if you experience more severe allergic reactions, which may involve face, neck, tongue, mouth or throat swelling, or difficulty breathing.
- Dry eyes from reduced tear flow (can be very troublesome if you use contact lenses)
- Inflammation of the liver (hepatitis), causing abdominal pain, loss of appetite and sometimes jaundice with yellowing of the whites of the eyes and skin and dark urine
- Reduced sexual performance (impaired erection)
- certain blood test results for liver function or fat levels differing from normal
- fainting
Very Rare: (may affect up to 1 in 10,000 people):
- Irritation and redness of eye (conjunctivitis)
- Hair loss
- Appearance or worsening of scaly skin rash (psoriasis): Psoriasis like rash.
* if treated for high blood pressure or angina then these symptoms occur especially at beginning of treatment, or if your dosage changes. They are generally mild or often disappear within 1 to 2 weeks.
Reporting of side effects If you get any side effects, talk to your doctor, pharmacist or nurse. This includes any possible side effects not listed in this leaflet. You can also report side effects directly: Website: www.zuventus.com and click the tab “Safety Reporting” located on the top end of the home page.
By reporting side effects, you can help provide more information on the safety of this medicine.
You can also report the side effect with the help of your treating physician.
5. How to store BisotrakTM
Keep out of reach of children.
Store below 30 ºC. Store in the original package in order to protect from light.
Do not use Bisoprolol Fumarate after the expiry date which is stated on the strips after EXP. The expiry date refers to the last day of that month.
Do not throw away any medicines via wastewater or household waste. Ask your pharmacist how to throw away medicines you no longer use. These measures will help protect the environment.
6. Contents of the pack and other information
What BisotrakTM contains
The active substance is bisoprolol fumarate.
Each film-coated tablet contains: Bisoprolol Fumarate 2.5 mg/5 mg
Packaging:
BisotrakTM 2.5mg: One Blister strips contains 10 tablets
BisotrakTM 5mg: One Blister strips contains 10 tablets
Marketing Authorisation Holder
Zuventus Healthcare Limited Zuventus House, Plot Y2, CTS No.: 358/A2, Near Nahur Railway Station, Nahur (W), Mumbai, 400078 Maharashtra, India
This leaflet was last revised in 06/2024
© Zuventus Healthcare Ltd., 2020. All rights reserved.